Credit: intermountainhealthcare.org
Researchers who have studied the effect of the body’s circadian rhythms on patients undergoing complex heart surgery have found that the time of day has an effect on the outcome of the surgery. Collecting data on nearly 600 patients who underwent aortic heart valve replacement over the course of six years, authors of a study recently published in Lancet found that patients who undergo open-heart surgery in the afternoon have better outcomes than those who have surgery in the morning. In the 500 days following surgery, patients who underwent afternoon heart surgery had half the risk of major adverse cardiac events (cardiovascular death, myocardial infarction, or admission to the hospital for acute heart failure) as those who had surgeries earlier in the day.
The team also conducted a randomized study of 88 valve surgery patients, half of whom had surgery in the morning, half in the afternoon. Researchers found lower levels of myocardial ischemia-reperfusion injury (tissue damage caused by blood supply returning to tissue in repaired areas of the heart) in patients who underwent heart surgery in the afternoon.
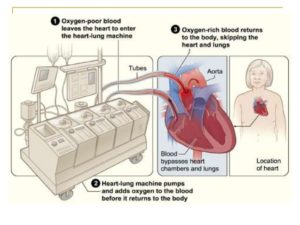
A heart lung machine oxygenates blood while doctors perform heart surgery. Tissue damage may occur when the blood is rerouted to the heart.
Credit: medgaget.com
The researchers took heart tissue samples from 14 morning surgery patients and 16 afternoon surgery patients in an effort to understand the reasons behind the different outcomes. When put in conditions replicating a heart refilling with blood, tissue from the afternoon surgeries recovered its ability to contract more quickly than the tissue from the morning surgeries. The researchers believe this discrepancy is linked to variation in gene expression in heart tissue throughout the day. The team identified close to 300 genes linking the body’s circadian clock to heart damage. A genetic analysis showed that these genes were more active in the afternoon than in the morning.
Blocking Gene Expression Improves Results
In a statement about the study, its lead author, University of Lille-France professor David Montaigne, said “There are few other surgical options to reduce the risk of post-surgery heart damage, meaning new techniques to protect patients are needed. Our findings suggest this is because part of the biological mechanism behind the damage is affected by a person’s circadian clock and the underlying genes that control it.”
Researchers tested the theory on mice by artificially removing or administering drugs that block the effects of the relevant genes. Mice given the drug or who had the gene removed recovered more quickly from morning surgeries. While further confirmation is needed to see if the findings translate to humans, the results indicate that developing drugs which target the relevant genes could help protect the heart during surgery.
Dr. John O’Neill, an expert in circadian rhythms from the MRC Laboratory of Molecular Biology, who was not involved in the study, says the study’s findings backed up research done on mice and fruitflies, which looked at genes’ involvement with the body clock. “The biological clock, the circadian rhythm, is in every single cell of the body, therefore it affects the biological activity of each cell type, commensurate with the function of those cells.” Dr. O’Neil also said that healthy hearts follow a pattern of activity throughout the day, and that in the morning the heart is not functioning at optimum performance.

 Heart Surgery May Be Best Performed In the Afternoon
Heart Surgery May Be Best Performed In the Afternoon


 Our Monthly Tip: Make an “In Case of Death” File to Ease Loved One’s Grief
Our Monthly Tip: Make an “In Case of Death” File to Ease Loved One’s Grief
















