If you’re a middle-aged woman and you live in the United States, you’ve had one mantra drummed into your head for as long as you can recall: “Get a mammogram once a year.” First introduced in 1976, mammograms have been touted as a life-saving screening technique for breast cancer for over 40 years. And, in fact, the number of breast cancer diagnoses has risen steadily during that time. Yet mounting evidence suggests that screening may very well be doing more harm than good.
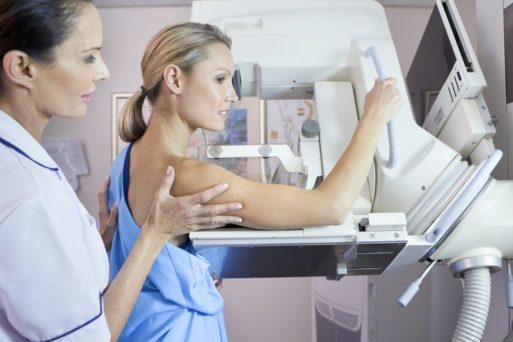
Credit: verywell.com
Now, the latest in a long string of studies questioning the value of routine mammograms has emerged. Published in the Annals of Internal Medicine on Jan. 10, 2017, the study, was conducted by researchers from the University of Oslo and Norwegian Institute of Public Health in Oslo, Norway. They found that “screening was not associated with lower incidence of advanced tumors,” and that one in three women diagnosed with early-stage breast cancer (also known as ductal carcinoma in situ, or DCIS) received unnecessary treatment, including mastectomy, lumpectomy, radiation and/or chemotherapy.
The researchers compiled their data by looking at the number of early-stage and advanced breast cancers detected by mammography before and after the country began offering free screening mammograms in 1979. In theory, if widespread screening was successful, the number of early-stage breast cancers detected would go up, while the number of advanced cancers would go down. In other words, detecting cancers early would prevent them from growing into large tumors, thus saving lives.
But what they found was that the number of early cancers detected by screening mammograms rose, but the number of life-threatening, late-stage cancers stayed the same. So, mammograms were catching cancers, but not necessarily the ones that needed to be caught.
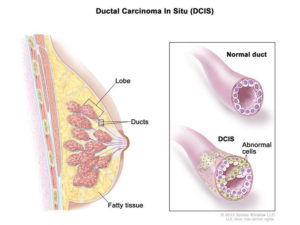
Ductal carcinoma in situ
Credit: cancer.gov
Surprisingly, the information in the Norwegian study is not at all new. Researchers have known for many years that screening mammograms detected many early cancers that might disappear on their own. But because the medical community can’t yet tell which of these early cancers will morph into a deadly one, the standard of care has been to treat them all.
“By treating all the cancers that we see, we are clearly saving some lives,” said Dr. Otis Brawley, chief medical officer of the American Cancer Society, when asked about the study in an interview with CNN. “But we’re also ‘curing’ some women who don’t need to be cured.”
Breast Cancer Deaths Declining, But Why?
Still, there’s no denying that the number of women dying from breast cancer has fallen steadily over the last 40 years. In 2013, the number of breast cancer deaths per 100,000 women in the United States stood at 21, down from 31 in 1975. In fact, advocates of regular mammograms, including the American College of Radiology, commonly use this statistic to support the contention that screening saves lives.
But that’s not necessarily true. In women under the age of 50, for example, screening has little value at all. Research shows that in order to save a single life, 2,000 women between the ages of 40 and 49 would need to be screened annually for over 10 years. During that time, six of those 2,000 women would ultimately die of breast cancer. Seven would die if there were no screening at all. Meanwhile, 20 out of the 2,000 women would receive treatment for breast cancers that would never have progressed.

Breast self-exam
Credit:bedfordbreastcenter.com
So if screening has little value, why are women surviving longer after a breast cancer diagnosis now than even 10 years ago? According to Tracy Onega, PhD, an associate professor of biomedical data science and epidemiology at Geisel School of Medicine at Dartmouth University, the answer is simple: Treatment has improved. Today, women who forego screening and discover they have cancer when they feel a lump have the same prognosis as those whose cancer was detected earlier on. And by waiting, they avoid the very real risk of being treated for cancer that would have gone away on its own.
Bottom Line: Screening for Cancer May Not Save Lives
We all want to believe that we have some control over our destinies. And the promise that cancer screening will help us live longer gives us some sense of control. But more and more evidence suggests that screening for most cancers doesn’t do much good.
Take, for example, prostate cancer screening, which the medical community touted as a superior means of catching and curing prostate cancer back in 1994. Despite the fact that, according to the doctor who invented the test, it is “hardly better than a coin toss” at detecting life-threatening cancers, it was the “gold standard” for prostate cancer screening for years. What’s more, like women with DCIS, men with even mildly elevated PSA levels were routinely subjected to prostate surgery, which is associated with serious complications, such as permanent impotence and urinary incontinence.
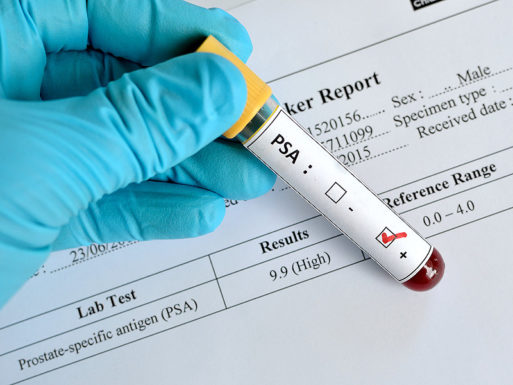
Credit: medscape.com
Still, before the American Urological Association finally stopped recommending routine screening for men under the age of 55 in 2013, 30 million men underwent PSA testing every year, at a cost of about $30 billion annually. Many of these men suffered long-term injury. Some died, and the number of deaths from prostate cancer did not decrease at all.
What to Do?
Cancer is a frightening disease, and one that almost everyone wants to avoid. For that reason alone, the decision to undergo screening for breast cancer or any cancer is a very personal one. So, speak to your doctor, and ask him or her to give you an honest evaluation of your actual risk. Then make up your own mind.
Meanwhile, there is much that each of us can do to lower our risk of breast and other cancers simply by altering our lifestyles. Check out this article from Prevention Magazine for some helpful tips.

 Do Mammograms Do More Harm than Good?
Do Mammograms Do More Harm than Good?


 Our Monthly Tip: Make an “In Case of Death” File to Ease Loved One’s Grief
Our Monthly Tip: Make an “In Case of Death” File to Ease Loved One’s Grief
 Passing of Beloved Comedian Births a New Comedy Festival
Passing of Beloved Comedian Births a New Comedy Festival















