America’s Life Expectancy Is Lowest in 20 YearsAmericans are dying younger today, and nobody is sure why
Life expectancy in the United States dropped for the first time in nearly two decades in 2015, according to a recent report from the National Center for Health Statistics. The […]
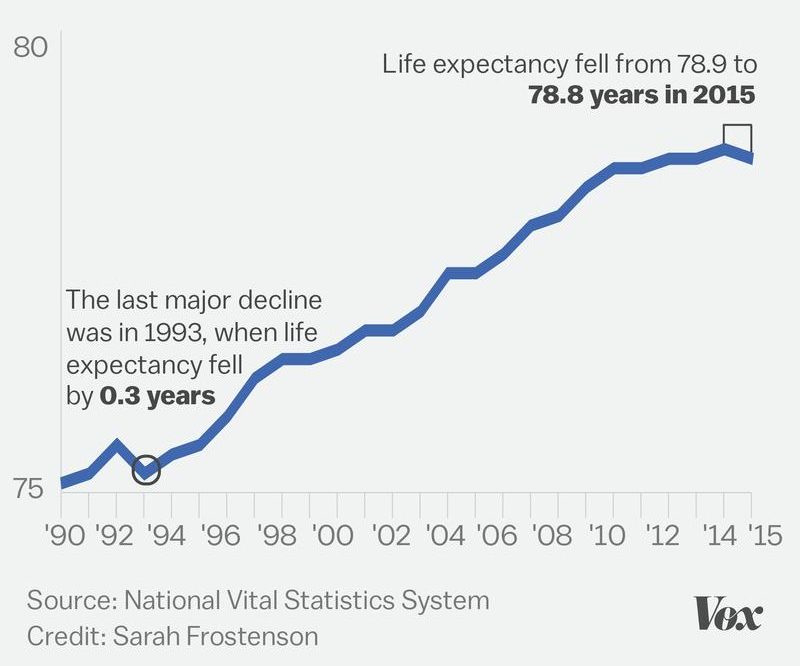
Life expectancy in the United States dropped for the first time in nearly two decades in 2015, according to a recent report from the National Center for Health Statistics. The decrease followed a several-year stretch in which the nation’s life expectancy stayed relatively flat after years of steady gain. The mortality rate also increased by 1.2 percent, from 724.6 deaths per 100,000 in 2014 to 733.1 in 2015.

The last time the country’s life expectancy fell was in 1993, during the height of the AIDS epidemic and a particularly bad flu season. There have been small, transient decreases in life expectancy in certain populations since then, said study author Jiaquan Xu. But this time the whole population is affected. And nobody is sure why.
Deaths from unintentional injuries — a category that includes drug and alcohol-related deaths and auto fatalities — rose by 3 percent during the period covered by the report. But this was not the only — or even the major — driver of the increase, according to Dartmouth health economist Jonathan Skinner. “Mortality is rising across a wide variety of illnesses. So it’s not just the opioid epidemic,” Skinner said in an email to Vox Media.
In fact, mortality rates for eight of the top 10 causes of death in the United States increased between 2014 and 2015, and infant mortality also rose. The only outlier was cancer deaths, which decreased by 1.7 percent. (The death rate from cancer has been dropping steadily over the past 20 years.)

The trend is particularly disturbing because many of these early deaths are largely preventable. Heart disease is still the top killer, followed by cancer and lower-respiratory diseases. “This is about poor health care and health behaviors — smoking, obesity, exercise, exposure to toxins,” said Philip Cohen, Ph.D., a health-inequality researcher and professor of sociology at the University of Maryland. “That means this is not about a failure of science to cure disease, but about people not having the wherewithal, or maybe the will, to take care of themselves and their family members.”
And while the increase in mortality among white, middle-class Americans has received a lot of press lately, the numbers show that life expectancy for both black and white men fell by about the same amount. Women fared slightly better, but their life expectancy decreased too. “That life expectancy hasn’t risen for any of the groups — black, white, Hispanic, male, female — is concerning,” Skinner said.
Have Americans Given Up?
The data on health outcomes is particularly concerning against the backdrop of stagnant wages and economic insecurity that has plagued much of the country since the Recession of 2008. Despite greater employment numbers, middle-class Americans have not seen their real wages increase in 20 years, and low-income workers’ wages have actually gone down. As a result, many people feel disempowered and helpless to improve their lives.
“My read is that this is related to stress, insecurity, and lack of self-efficacy,” Dr. Cohen said. “That is, people don’t know what their future holds, they have no confidence that their lives will move in a positive direction, and they don’t feel they are in control of their own destinies. That is what leads to self-destructive behavior.”

Credit:blog.maryfons.com
If Cohen is right, it’s possible that things may get much worse. The Trump administration has promised to dismantle much of America’s safety net and repeal the Affordable Care Act, which provided free preventive care and coverage for pre-existing conditions to millions of Americans. And the much-touted 21st Century Cures Act, which was approved by the legislature in December 2016, is being paid for with $3.5 billion in cuts to public health programs, which is exactly where the country needs to focus if Cohen’s assessment is correct. In fact, focusing on curing disease rather than changing health behaviors is “missing the importance of addressing the behavioral factors in health that are most likely driving the rise in mortality,” Skinner said.












Leave a Reply