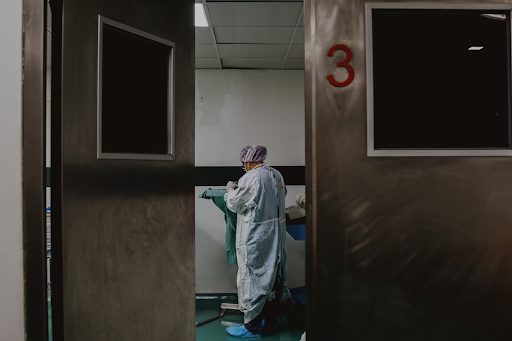
While most physicians indicated that they would not prefer invasive treatments regarding end-of-life care, these same treatments are routinely administered to their patients.
Credit: sjobjio on Unsplash
A 2025 international study published in the Journal of Medical Ethics and reported by Medscape revealed a surprising disconnect in end-of-life care for physicians between what they offer patients and what they’d choose for themselves. While most physicians indicated that they would not prefer invasive treatments regarding end-of-life care, these same treatments are routinely administered to their patients.
In the recent study, researchers surveyed 1,157 physicians from countries including Belgium, Italy, Canada, the United States, and Australia about their personal preferences involving end-of-life healthcare and life-prolonging treatments. The findings may indicate what happens when advanced medical training meets mortality.
When asked what treatments the physicians would want for themselves if diagnosed with advanced cancer or Alzheimer’s disease, they rarely considered life-sustaining practices a good option. Only 0.5 and 0.2 percent would choose cardiopulmonary resuscitation (CPR), 0.8 and 0.3 percent for mechanical ventilation, and 3.5 and 3.8 percent opted for tube feeding for cancer and Alzheimer’s, respectively. A staggering half of physicians surveyed preferred euthanasia if it were legally available for both diseases. 90% would opt for symptom-relieving treatment instead, and 95% would decline CPR, mechanical ventilation, and tube feeding entirely.
Medscape notes that patients continuing to receive treatments that these physicians would decline “highlights a striking disconnect.”
“Globally, people are living longer than they were 50 years ago. However, higher rates of chronic disease and extended illness trajectories have made end-of-life care an issue of growing clinical and societal importance,” the researchers, led by Sarah Mroz, PhD, wrote.
There are complex pressures at play within the modern healthcare system. Doctors operate within a healthcare system that measures success as pursuing every option available and requested by patients and families. Many physicians may also fear legal consequences; choosing restraint may be construed as negligence.
Physicians have in-depth knowledge of, and training about, the extent of invasive medical procedures and their impact on quality of life. When facing their own mortality or that of loved ones, they tend to focus on quality of life over prolonging it as long as possible. When it comes to patients, these dynamics tend to shift.

Physicians have in-depth knowledge of, and training about, the extent of invasive medical procedures and their impact on quality of life.
Credit: National Cancer Institute on Unsplash
Local culture and geography play a role in physicians’ end-of-life preferences as well. For those practicing in jurisdictions where euthanasia and medical aid in dying are legal, they were three times more likely to consider euthanasia for cancer and twice as likely regarding Alzheimer’s disease. In Belgium, 80 percent of physicians would consider euthanasia for themselves; assisted dying has been legal since 2002. In the US state of Georgia, however, preference for euthanasia was just over 37 percent; assisted death is not legal in this jurisdiction.
An avoidance of death in Western societies may also play a role in the gap between physicians’ end-of-life preferences versus what they recommend for their patients.
“In many Western societies, death is still seen as a failure—even in medicine,” Andrea Bovero, a psychologist interviewed by Medscape, explained. “This mindset contributes to the avoidance of honest conversations about dying and a preference for treatments that delay or deny death.”
As a result, physicians have to balance societal expectations and their training.
This journey is wonderfully highlighted in Atul Gawande’s book Being Mortal. Gawande, an endocrine surgeon, reflects on his personal experiences and cultural practices surrounding elders and end-of-life care, combined with his perspective as a physician.
As populations age and chronic diseases extend health complications, the need for compassionate end-of-life care has only grown. Bridging the gap between what doctors would choose for themselves and what they offer patients could be one of the keys to a healthcare system that prioritizes listening, support, and quality of life.

 Recent Study Shows Physicians Choose Much Different Treatment Options for Themselves vs. Their Patients
Recent Study Shows Physicians Choose Much Different Treatment Options for Themselves vs. Their Patients


 Final Messages of the Dying
Final Messages of the Dying
 Will I Die in Pain?
Will I Die in Pain?















