 In its May 1, 2025 issue, Science magazine published a research article written by neurologists and a bioethicist discussing the potential research benefits — and the subsequent delicate ethical considerations — of using “physiologically maintained deceased” organ donors, or PMDs, for research into new drug therapies.
In its May 1, 2025 issue, Science magazine published a research article written by neurologists and a bioethicist discussing the potential research benefits — and the subsequent delicate ethical considerations — of using “physiologically maintained deceased” organ donors, or PMDs, for research into new drug therapies.
As the team explains, PMDs are “deceased humans in whom ventilation and circulation are maintained for a defined period after the declaration of death by neurologic criteria (brain death), [and therefore] mimic live human physiology.”
The use of PMDs in the early stages of medical research for drug therapies could potentially advance important studies much more quickly, efficiently and effectively, the authors of the article argue.
The authors of the Science paper touch on two points: Fundamentally, the difficulty lies in establishing appropriate guidelines regarding how PMDs are used, and devising communication methods for explaining the process to people who aren’t in the medical research field.
The authors also propose the idea of using whole bodies for research in a new way: to discover and test new drug therapies.
As a science reporter at El Pais summarizes the article, the researchers “propose using the bodies of brain-dead people in hospitals to carry out medical experiments to advance research into treatments for currently lethal diseases.”
PMD-Based Research Raises Important Ethical Questions
While the use of whole bodies of deceased people sounds like a relatively straightforward medical concept, the ethical complications surrounding the process can be staggering.
One issue is that many people are uncomfortable with brain death being the determining factor of whether someone is alive or dead. Brain death is defined in part as “the irreversible cessation of all functions of the entire brain, including the brain stem.”
It is the standard legal definition of death; it means that the individual will not regain consciousness or be able to breathe without mechanical assistance. Again, that seems pretty clear-cut, but an article published by Johns Hopkins Medicine presents it in such a way that might make you think twice:
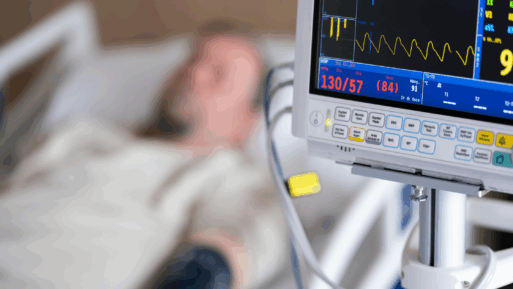
“A woman lies in a bed at the … hospital. Aided by a ventilator, her lungs inflate, deflate, and fill again. Her heart beats and her skin is warm. But her eyes stay closed and she does not react to stimuli such as pain and light. Is she alive or dead?”
The problem lies in the fact that medical technology has advanced to such a stage that it makes it difficult for some to accept brain death as dead.
Although brain death is distinct from a coma or vegetative state, many nonmedical people have a hard time distinguishing among the three, and that could make some people — and their decision-making family members — reconsider opting for whole body organ donation. It is one thing to feel as if your recently deceased loved one is being “kept alive” just long enough to undergo the surgery required for organ donation; it’s another to picture them continuing to lie in their hospital bed while medical research is being performed on their seemingly alive bodies.
Additionally, when people register as organ donors, it is often with the presumption that their donation would go toward living recipients, that is, transplantation of organs. The authors note that research purposes might not have been a consideration. This makes research on PMD bodies a touchy gray area. As the authors write, “Consensus around brain death rests at the core of the ethical justification of PMD-based research.”
PMD-Based Discovery Research versus Late-Stage Studies
The scientists who authored the Science article explain that as of today, PMD research has already been critical in enabling “quasi- ‘first in human’ studies without posing risk to living patients.” This kind of research has led to breakthrough medical achievements like the recent successful xenotransplantation — the transplanting of genetically modified animal organs into living human patients.
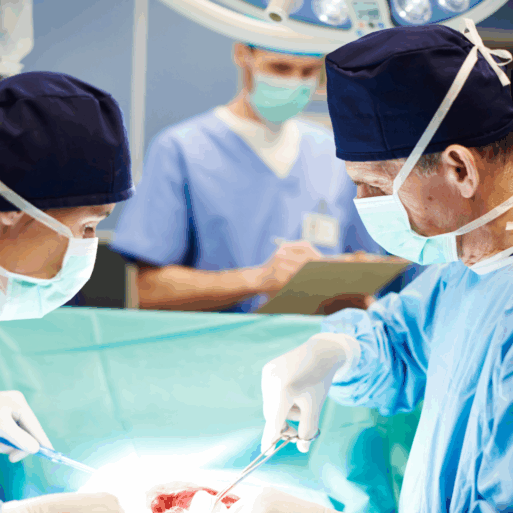
Genetically modified animal organs have been successfully transplanted into humans using research done, at least partially, on PMDs
Other advancements that have come from the use of whole bodies to conduct research includes the integration of gene editing and bioengineering techniques, which have helped overcome some common complications involved with post-transplant organ rejection.
In the recent article, however, the scientists pitch a slightly different use of PMDs: to discover and test new human drug therapies.
They propose that there is enormous potential for PMD-based research to substantially enhance the scale and efficiency of therapeutic discovery research — that is, the initial phase of drug development that focuses on identifying and validating new drug targets, as well as potential therapeutic compounds for treating diseases.
The authors recognize that this type of research might not be an incentive for donors or their families, because the immediate benefits aren’t as obvious. While would-be whole body donors more easily understand “the benefits of late-stage studies such as xenotransplant,” they write, “by contrast, the benefits of early-stage therapeutic discovery research are less tangible or proximate, and this may affect the next of kin’s decision-making.”
In other words, many people find comfort knowing that their loved ones’ death was able to give new hope to a living patient when they are able to donate an organ or tissue. But there might not be much immediate comfort to be gained from these initial phases of research into drugs, making PMD-based studies a hard sell to bereaved family members.
Strict Guidelines and Protocols Are Needed
In addition to addressing the acceptance of brain death and the proper treatment of human remains, the scientists outline five different aspects they feel should be clarified — and potentially differentiated from those governing single-organ donation — to avoid potential abuses or mischaracterizations of whole body organ donation.
- General Ethical Priorities: Maximize respect for the deceased, minimize emotional and/or moral harms to their loved ones or next of kin and preserve public trust.
- Eligibility for Research Participation: Donation for transplant (as opposed to whole-body PMD donation) should take precedence over donation for research. Establish guidelines for ensuring that neither the deceased nor their family members would be opposed to PMD-based research for any reason. (For example, they may need to differentiate organ donation registry to specify between organ donation for transplantation, and whole body donation.)
- Consent and Informed Authorization: Provide full disclosure of meaningful information about PMD research to whoever is making the decisions for the deceased. Brain death is rarely something that can be predicted in advance, and isn’t something likely to be outlined in a living will or medical directive statements).
- Impacts on Facilities and Personnel: Make sure any PMD-based research isn’t occurring in such a way that it detracts resources – such as staff and medical equipment – away from living patients in intensive care units (where such research would often be undertaken.)
- Oversight and Accountability: Implement policies to ensure close review and approval of PMD research by review boards or appointed committees.
They hope that by carefully deliberating ethical guidelines in advance of any research using PMDs, establishing clear language, and increasing community engagement to establish a better understanding of a complicated scientific procedure, could have researchers going down the right path, ultimately offering “tremendous potential for advancing science.”

 Whole Body Organ Donation Raises Ethical Considerations
Whole Body Organ Donation Raises Ethical Considerations


 Final Messages of the Dying
Final Messages of the Dying
 Will I Die in Pain?
Will I Die in Pain?















