Today SevenPonds speaks with Dennis Kowalski, a nationally registered EMT-Paramedic for the city of Milwaukee, Wisconsin. In the field, Dennis frequently encounters emergency medical situations, and has years of experience attending to those in crisis. In addition to his work as a paramedic, Dennis also works as a firefighter, an instructor at the Milwaukee Fire Academy and as the director of Cryonics Institute (a non-profit organization specializing in cryopreservation after death).
Note: This interview has been edited for length and clarity.

Credit: Dennis Kowalski
Marissa Abruzzini: Thank you for speaking with us! Let’s start with your background. When did you become a paramedic, and what made you get into this line of work?
Dennis Kowalski: It started about 14 years ago, with the fire department. I thought that being a firefighter was exciting, but I wanted to use my mind more deeply. As a paramedic, you need to have a deeper understanding of medicine and trauma. In other words, you need to have a bigger tool chest in order to have a positive impact. The EMT (Emergency Medical Technician) training that you receive as a firefighter is very basic. There’s really only so much firefighters can do. Paramedics can do more in emergency medical situations. They can administer more drugs; they can manage the patient’s airway, and they need to understand how to access veins for IVs. Paramedics are like the hands and eyes of the doctor in that sense.
Marissa: As a firefighter and a paramedic, I’m sure you deal with plenty of emergency medical situations in your line of work. Are some of these cases harder to deal with than others?
Dennis: I have a special place in my heart when dealing with brain diseases like cancer and dementia. Recently, about five years ago, my father lost all of his mental faculties. Contrary to what you might think, this can actually be harder than dealing with someone who dies quickly. Sure, with these degenerative diseases you get to say goodbye, and there’s some closure there. But then there’s the suffering aspect. You have to watch as someone loses their faculties. This is why, personally, I’d rather go quickly.
Marissa: How do you deal with these situations in the field?
Dennis: When I see this as a paramedic, especially when family members are there, I educate them, and I also provide comfort to them. One of the biggest problems that I encounter is that many people don’t prepare for emergency medical situations like this. They may have outdated insurance information that leaves their entire life insurance policy to an ex- spouse, for example. It happens a lot, more than you would think.
Another problem in cases like this is that DNR (Do Not Resuscitate) orders aren’t explained or understood properly. I’m often out in the field trying to explain to people how the hospice process works. People are so afraid of hospice care. They don’t realize that it can be done in their own home, and that there are resources out there for dementia, brain cancer and other diseases that cause you to lose faculties. All of this can be difficult to explain during an emergency.

Credit: Wikimedia.org
Marissa: I can imagine that would be hard. How often do you come across people who have a DNR order in place?
Dennis: There are so many people who don’t have DNR orders, but should. And the ones who do have a DNR in place usually have something important missing in the paperwork. We’ll muddle through it as best we can. But I’ve noticed that a lot of people want to sweep it under the rug. They don’t want to think about it, and so they don’t have one.
Marissa: How do paramedics deal with DNRs? What steps are you allowed to take in an emergency, and what steps are you not allowed to take?
Dennis: It can be complicated. Someone might say they have DNR, but if they don’t have the bracelet and paperwork, there is a possibility that we will work on them anyhow. We always default to CPR. Usually, if there’s a family member there, I’ll try to get the family doctor on the line right away, and in the meantime, I’ll start CPR. The thing is, even if we start CPR, we can end it right away if we find out that the person has a DNR.
When you have a DNR order, you’re actually told not to call 911 unless there are very specific things that we, as paramedics, can do. So, we can give oxygen to make the person feel more comfortable, for example. But there are many things that we can’t do if there’s a DNR.
Marissa: What can people do to better prepare for emergencies like this? What steps can they take to improve their chances of survival, and to make a paramedic’s job easier?
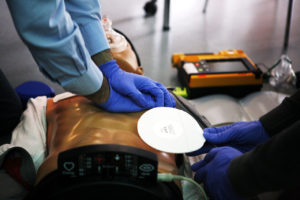
Credit: Wikimedia.org
Dennis: A lot of times they call professionals and expect them to take care of it. But you have to prepare for these emergency medical situations ahead of time. It’s important to ask questions and speak with knowledgeable healthcare advocates. Look up living wills, hospice care and DNR orders. Ask your doctor, or the nurse, or someone who has expertise about these details. Fill out your paperwork. There are a million resources, so all you have to do is ask questions, talk, and prepare. Make sure everyone is on the same page. As I said, we default to CPR a lot of times, so if this is something that you absolutely don’t want, then you need to make the preparations now.
One of the best things I’ve seen in the field lately is a File of Life. It’s a magnet with information on it that summarizes all of your medical needs (including DNRs and medications). Paramedics can immediately see which medications you’re taking, who your primary care doctor is, how to contact your doctor, and what your wishes are. You can put it on the refrigerator door. They even have stickers that you can put somewhere in your car. You can put it anywhere that EMTs, police officers and firefighters can easily access it. This makes it so much easier to handle emergencies, especially when things are emotional. Your wishes will be honored, and the paramedics will know exactly what to do.
This concludes part one of my interview with Dennis Kowalski. Please join us next week when we discuss how cryopreservation works, and the role that paramedics play in cryonics.

 How Can We Better Prepare for Emergency Medical Situations?
How Can We Better Prepare for Emergency Medical Situations?


 Our Monthly Tip: Make an “In Case of Death” File to Ease Loved One’s Grief
Our Monthly Tip: Make an “In Case of Death” File to Ease Loved One’s Grief
 Passing of Beloved Comedian Births a New Comedy Festival
Passing of Beloved Comedian Births a New Comedy Festival
















Interesting interview. I have always wanted to know more about a paramedics perspective. Looking forward to Part 2.
Report this comment