Today SevenPonds speaks with Irene Smith, founder and director of Everflowing, an educational program centered around creating a more supportive environment for hospice patients and their healthcare providers. Smith has three decades of experience as an educator and practitioner, focusing primarily on the benefits of touch at the end of life. As an author, she has also published a number of works, including “Touch Awareness In Caregiving,” “The Emotional Impact Of Working With The Dying” and “Providing Massage in Hospice Care.” Today, her goal is to teach others how to perform mindful touching and to bring a sense of humanity back into the healthcare profession.
Editor’s note: This interview has been edited for clarity and length.
 Marissa Abruzzini: Thank you for joining us, Irene. Let’s start with your background. What inspired you to get involved in this work?
Marissa Abruzzini: Thank you for joining us, Irene. Let’s start with your background. What inspired you to get involved in this work?
Irene Smith: I originally received a massage license in 1974, but I put it to no therapeutic use at the time. That was until I met Elisabeth Kübler-Ross in 1978. I spent a year working with her and learning from her, and at the end of my time, she wrote me a reference letter, and encouraged me to work with the dying with my massage therapy. I decided to take my massage practice to a hospice facility in 1981, by offering massage to people who were dying.
Marissa: Was there any specific certification for this work at that time, or was this a brand new field?
Irene: They actually only introduced this as a specific modality in massage about four years ago. There was absolutely nothing like it when I began. And this practice was a difficult one to pioneer, because the AIDS epidemic was just beginning. So many people at the time refused to give education or training on massage for people who had HIV/AIDS. In 1982, I founded a non-profit called Service Through Touch, which offered therapeutic massage to people around the world who have HIV/AIDS. But this type of service was still largely ignored for about 18 years.
It wasn’t until after the AIDS epidemic that massage in hospice became more mainstream. Oncology in particular was what made it mainstream. People who were on hospice care began receiving massage as part of their cancer treatments. And today, most major healthcare corporations have massage teams on-staff.
But, massage is not the intention of my work today. My work goes much deeper than massage. My real work is as a touch educator, not a massage therapist.

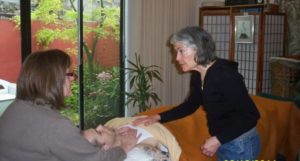
Irene and Evee Mills, Zen Hospice Project, 2010, Photo by Alan Waugh
Marissa: Tell me more about that.
Irene: Today, massage has become a corporate modality of care, which has been incredibly wonderful for many people. But healthcare professionals need to understand that their quality of touch is the core vibration that every patient responds to. Whether they’re bathing someone, or transferring someone from one bed to another, nurses and doctors are often taught to touch patients as little as possible. Touch isn’t included in any paradigm.
So, my mission is to assist healthcare providers and family to recognize the value of the care that they provide. I want to show them that they don’t need to separate entirely from the people they care for. They need to learn how to touch skillfully. And this benefits everyone in the process. Right now, about 85 percent of the time, healthcare providers are working with people without having training on this necessary core skill. They need to appreciate the value of touch.
Credit: Irene Smith/LinkedIn
Marissa: Interesting! How do you teach caregivers this skill?
Irene: I actually just came back from Connecticut to train 14 staff members on touch awareness. When I teach someone about touch awareness, the most important thing to remember is that touch isn’t really a “technique.” It’s more like an all-encompassing sense. Touch has power beyond the physical. Let me give you an example; if someone loses the opportunity to form coherent sentences, this causes a gap in communication. With touch, this person can bridge the gap between despair and hope. They can communicate without using words.
The main problem with how healthcare providers treat touch today is that they move too fast, or in an unskillful way that tells their patients “I don’t have time for you.” This produces anxiety in people. The provider may not understand that their touch is a delivery system, and that it holds value. There is value in just holding someone’s hand. Sometimes, it takes a full year to gather the confidence to perform just one act of human kindness like that.
This concludes the first part of our interview with Irene Smith. Join us again next week for part two of our interview, where we talk to Irene about the benefits of touch, and how all of us can become better caregivers.

 How Important is Touch at the Bedside of the Dying?
How Important is Touch at the Bedside of the Dying?


 “The Boy and the Heron” by Hayao Miyazaki
“The Boy and the Heron” by Hayao Miyazaki
 Honoring Seniors, Caregivers: Inside the Vision of Carehaus
Honoring Seniors, Caregivers: Inside the Vision of Carehaus
 “In Case You Don’t Live Forever” by Ben Platt
“In Case You Don’t Live Forever” by Ben Platt















I am a massage therapist and recently walked a dear friend through death. It was precious in that it involved a lot of touch.
Report this comment
I am a massage therapist, an End of Life Doula and a retired R.N with more than 30 years experience in both acute hospital, ICU, E.R and palliative home care. When I entered nursing, we were taught to put our hands on our patients, to feel their skin,their temperature, their pulse. With the advances in medical technology- hands on is not required to “ see what is going on”.
The Art of human touch is a skill that is easily learned and shared.
I am grateful and thankful for this.
Report this comment
So glad you appreciated this article. Thank you very much for your feedback.
Report this comment