Today SevenPonds speaks with Irene Smith, founder and director of Everflowing, an educational program centered around creating a more supportive environment for hospice patients and their healthcare providers. Smith has three decades of experience as an educator and practitioner, focusing primarily on the benefits of touch at the end of life. As an author, she has also published a number of works, including “Touch Awareness In Caregiving,” “The Emotional Impact Of Working With The Dying” and “Providing Massage in Hospice Care.” Today, her goal is to teach others how to perform mindful touching and to bring a sense of humanity back into the healthcare profession.
Editor’s note: This interview has been edited for clarity and length.
 Marissa Abruzzini: You train healthcare professionals and caregivers on touch awareness. How does this training benefit the people that they work with?
Marissa Abruzzini: You train healthcare professionals and caregivers on touch awareness. How does this training benefit the people that they work with?
Irene Smith: Well, there are a number of benefits that people will notice. Some are scientific. For example, as we experience the sensation of touch, a hormone called oxytocin is released. This lessens anxiety, and promotes feelings of bonding. Touch can also release powerful endorphins in the body, which help balance out pain with pleasure.
But beyond the release of these hormones, touch also helps with proprioception. This is essentially an energy or state of being that allows us to understand where our bodies are in space. Touching increases this. It’s such a powerful thing to witness. When touching someone who has been in bed for months, you have the opportunity to watch their body parts remember where they are in space for the first time in days or weeks. This is especially important for people who have Huntington’s, Lewy body dementia and other diseases which cause bodies to lose control.
Marissa: And what about the psychological impact?
Irene: Touch promotes powerful feelings. I’ve watched people remember their loveliness, and it’s a beautiful thing to see. I’ll give you an example. When I put lotion on someone’s hands for just five minutes, working slowly, gently and mindfully, when I am finished, nine times out of 10, that person will hold their hands in front of them and stare at them in awe. They have tears in their eyes, because they’re remembering how beautiful their hands are, and how lovely they feel. Touch becomes an emotional language.
Credit: Irene Smith/LinkedIn
I’ve found that there are usually deep feelings beneath someone’s diagnosis that sometimes they’re not even aware are there. There’s a strong desire for autonomy, hope and a need to connect to the world in a meaningful way. By focusing on touch, I’ve seen improvements in self-esteem. They often feel better about themselves knowing that someone is taking the time to really be with them, in the moment. They feel worthy of being cared for.
Marissa: Do you ever find this work emotional for yourself as well?
Irene: Sure! The great thing about touch awareness is that we give permission for caregivers to be human. My peers understand that it’s OK to share a vulnerability — we give permission for that. Touch was never meant to be a luxury for people; it’s a basic human need. And this is true for both the caregiver and the receiver. Touch is the integral thread that forms the essence of comfort care. Validating that touch isn’t something that’s outside of what we’re already doing.
Marissa: How difficult is it to learn better touch awareness skills, as a caregiver?
Irene: The most important thing to remember is that this is an organic language that we’re born with — it allows us to establish a relationship with ourselves and the world from the start. Before we’re even taught basic dialect, we interact with the world through touch. So caregivers and the people they work with are really just getting back to that core communication. At the end of life, many people aren’t capable of speaking. That form of communication is no longer available to them. Touch bridges this gap.
Marissa: What are some of the challenges that caregivers face when they learn about mindful touch awareness?

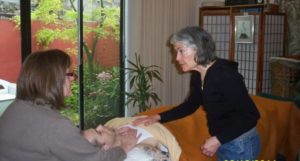
Irene and Evee Mills, Zen Hospice Project, 2010, Photo by Alan Waugh
Irene: Our healthcare profession is steeped in this idea that touch is completely outside of what they’re doing when they’re around patients. In this country, touch is mostly associated with intimacy. It becomes a dirty word, or something sexual. In reality, touch is just a very basic form of human language.
This idea is very hard to let go of for some caregivers. I’ll give you a great example of this. About three months ago, I was training a group of caregivers about touch awareness. One nursing student came up to me after the presentation and said, “That was an absolutely wonderful presentation! But my professor says that we should never touch our patients.”
I responded, “Please tell me, do you dress or undress them?” The nursing student says, “Yes, sometimes.” So, I asked her, “Can you demonstrate how to do that without touching the patient?” This conversation went on and on. “Do you ever give medication to a patient? Do you take their blood pressure? How do you do any of that without touching the patient?”
It’s so ingrained in our healthcare system that nothing caregivers or doctors do is touching. This is a major hurdle to get over because in reality, everything is touching. I’m trying to get people to understand that, and to be more aware of it. My goal is to leave a legacy that others can follow. I see a missing link in the healthcare paradigm, and I want to serve the world through this compassionate work.
If you missed part one of our interview with Irene, please catch up here.

 How Does Touch Awareness Improve Caregiving and Healthcare?
How Does Touch Awareness Improve Caregiving and Healthcare?


 “In Case You Don’t Live Forever” by Ben Platt
“In Case You Don’t Live Forever” by Ben Platt
 Our Monthly Tip: Make an “In Case of Death” File to Ease Loved One’s Grief
Our Monthly Tip: Make an “In Case of Death” File to Ease Loved One’s Grief
 Passing of Beloved Comedian Births a New Comedy Festival
Passing of Beloved Comedian Births a New Comedy Festival














