Today SevenPonds is speaking with Dr. Jessica Nutik-Zitter, M.D. Dr. Zitter is a board certified specialist in both critical care and hospice and palliative medicine and an attending physician in the intensive care unit at Highland Hospital in Oakland, California. She was featured in the award-winning Netflix documentary “Extremis” and is the author of the recently released book “Extreme Measures: Finding a Better Path to the End of Life.”

Dr. Jessica Nutik-Zitter
Kathleen: Thanks so much for speaking with me today, Dr. Zitter. I’m very excited to hear about your work.
Dr. Nutik-Zitter: My pleasure, Kathleen.
Kathleen: Can you start out by telling me a little bit about your dual role at Highland Hospital?
Dr. Zitter: Certainly. I work both as an attending physician in the Intensive Care Unit and as an attending physician on the palliative care team. When I am attending the ICU, I direct the care of all of the patients in the ICU. At other times, I function primarily as a palliative care consultant. For instance, I may be asked to help the ICU team manage a patient’s pain, or address goals of care with a patient who is not doing well despite aggressive efforts to save his or her life.
Kathleen: Some people might see critical care and palliative care as somewhat contradictory specialties. How would you respond to this?
Dr. Zitter: My goal is to help people see that these are not at all disparate roles but part of the continuum of patient-centered care. When a patient first presents in the Emergency Room or Intensive Care Unit, it’s appropriate, in most cases, to make every effort to stabilize them in the hopes of restoring them to their former state of health and quality of life. But for many patients, continuing aggressive intervention when it doesn’t appear to be helping and may actually be harming them is not in their best interests. At that point, it’s equally as appropriate to take a different approach.
Kathleen: Can you tell me what you mean by the “end-of-life conveyor belt?”
Dr. Zitter: Sure. The end-of-life conveyor belt refers to the use of ICU tools and technologies for patients who will not benefit from them or for whom the potential benefits don’t outweigh potential harms. Unfortunately, most people who land in the ICU receive all of these aggressive therapies by default, even when they are clearly not doing any good.
Kathleen: How does this “conveyor belt” get started?
Dr. Zitter: That’s a good question! I believe it starts with our cultural denial of death. We are all chasing the mutual fantasy that we can stay alive forever. And the advances in medicine and technology over the last 50 or so years created a perfect storm that allows us to keep that fantasy going. As long as there’s another medicine or another intervention to try, we can pretend death isn’t inevitable even when it clearly is.
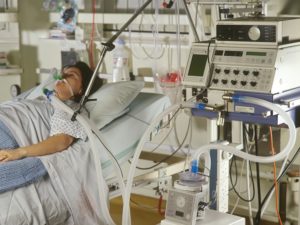
Credit: nursingtimes.net
Kathleen: Is there a way to stop it? Once a patient is admitted to the Intensive Care Unit and doctors have started interventions like breathing tubes, ventilators and blood pressure support, how can you scale back?
Dr. Zitter: I believe that the answer to that is communication. For doctors, that means being willing to break bad news — to tell the patient and/or his family that the things we are doing are not working, and it’s time to reassess goals of care. For patients and their loved ones, it means being open to the truth. That can be very hard, especially after many days or even weeks of a “full court press.” But these conversations are essential. We need to talk about the kind of care the patient wants (or his family believes he would want) as he approaches the end of life.
Kathleen: Do you think it’s possible to prepare for these kinds of situations in advance? For example, if a patient has a terminal illness, are there steps they can take to avoid the ICU?
Dr. Zitter: Again, this is where communication is key. We should all be talking to our loved ones about how we want to live at the end of our lives and how we want to die. This is especially important for people who have a life-limiting illness. The time to have the conversation about preferences is not when the person arrives at the hospital in acute distress. At that point, the conversation gets hijacked by the urgency of the situation, and care may be initiated that the patient really doesn’t want.
This concludes Part One of our interview with Dr. Nutik Zitter. Please join us next week for Part Two.

 How Can Palliative Care Be Implemented in the ICU?
How Can Palliative Care Be Implemented in the ICU?


 “In Case You Don’t Live Forever” by Ben Platt
“In Case You Don’t Live Forever” by Ben Platt
 Our Monthly Tip: Make an “In Case of Death” File to Ease Loved One’s Grief
Our Monthly Tip: Make an “In Case of Death” File to Ease Loved One’s Grief
 Passing of Beloved Comedian Births a New Comedy Festival
Passing of Beloved Comedian Births a New Comedy Festival















This is so timely: I’ve been contacted by an ICU doctor (from one of the largest health centers in Canada). His idea was to bring seniors into the ICU and have a convo after. My recommendation: show Extremis in Retirement/Seniors Residences .. and have a convo after. 🙂
Report this comment
Great idea!!
Report this comment