Credit: acco.org
Over the past two decades, the medical specialty of palliative care has exploded in the United States. And with it, the understanding of what palliative care is and to whom it should be offered has evolved considerably. As recently as 10 years ago, most doctors equated palliative care with end-of-life symptom control. Today, however, a growing number of physicians have come to understand that “palliation” is a philosophy of care that helps patients and their families achieve the best possible quality of life, no matter where in the trajectory of their illness they may be.
Now, at pediatric hospitals like St. Jude’s Children’s Hospital in Memphis, Tennessee, that philosophy is reaching some of the youngest and most vulnerable patients: children with cancer. Through a program led by Dr. Justin Baker, St. Jude’s director of the Quality of Life and Palliative Care Division, the hospital is offering pediatric palliative care to every child who receives a cancer diagnosis from Day 1.
The Challenges of Treatment
A cancer diagnosis is terrifying for a child. Although very young children are unable to grasp the full reality of their illness, research shows that children as young as 3 know when they are very ill, according to a recent report in the New York Times. At the same time, they are too young to understand why they must endure painful and debilitating treatments aimed at curing their disease. And they lack the psychological resources they need to cope.
Older children may have a better intellectual understanding of their diagnosis and treatment plan. Yet they are no more prepared to handle the enormous stress and distress that undergoing treatment for cancer creates. What’s more, they have a much better understanding of the concept of mortality. They know that it’s very possible they may die from their disease. And that’s a lot to handle when you have only a handful of years under your belt.

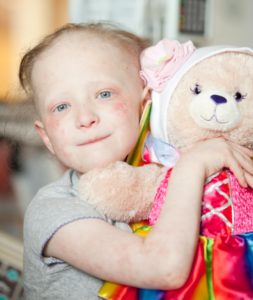
Mia S. has Ewing’s sarcoma, a pediatric cancer
Credit: YouTube
Helping Kids Cope
The Quality of Life and Palliative Care program at St. Jude’s aims to address the unique needs of children with cancer in direct and age appropriate ways. For example, someone from the team greets every child admitted to the service with a koala-shaped “stress ball” and explains to them that they should squeeze it when they feel frightened or upset. The koala (a loose homonym for QoLa, an acronym for “Quality of Life for All”) also sports a phone number on its bottom. The staff tells each child that they can use the number anytime for any reason if they need help from the staff.
That help can come in many forms. For young children it may be opportunities to communicate their distress through play therapy, music or art. For older children, it may be the chance to talk to an empathetic adult — someone they need not “protect” from the negative emotions they feel. (Children often hide these feelings from their loved ones in an effort to shield them from more pain.) And for dying children, it may mean having the chance to express what they want the rest of their lives to look like, and what they hope for as life comes to a close.
Even “mundane” issues such as scheduling appointments or giving medications to a toddler can be very stressful for families dealing with a sick child. So the team also works with parents and other caregivers to help in these areas as well. And while the palliative care team leads these efforts, all staff at the hospital get training in palliative care. And anyone can offer a helping hand.
A Model for the Future
In June 2017, St. Jude’s held its first Pediatric Palliative Oncology Symposium. It was attended by over 300 doctors, nurses, and psychosocial professionals who came from 33 states and 19 countries to learn how pediatric palliative care is implemented at St. Jude’s.

Credit:blogs.rch.org.au
One of the highlights of the symposium was an interactive role-playing session with parents of children who had died several years before. These parents have been deeply involved with the pediatric palliative care program at St. Jude’s from its outset. And one of their major goals has been to help doctors and other healthcare professionals learn how to communicate more effectively with families. Thus, involving them in the symposium was a big plus for all concerned.
“To have the parents here interacting on the ground was really wonderful and valuable,” said Dr. Aimee Thompson, a psychologist with Cincinnati Children’s Hospital in a statement to the Memphis Daily News. “At our table we had people from a number of different disciplines, so to hear different perspectives and to learn from one another was really important.”
Yet another session at the conference explored the benefit of music therapy for children who are dying. Said Dr. Baker, “When Amy [Love, St. Jude’s music therapist] comes into a room and is able to provide really beautiful music therapy, everything just slows down. There is deeper breathing, less pain, and the room calms down as a whole,” he said.
Not Just for the Dying
But Baker also emphasized that pediatric palliative care is not just for children who are dying. “More than 60 percent of the patients we see have a primary goal of cure at this particular point,” he said. “We’re much more about a true quality-of-life team where our motto and the whole purpose of our being is to help every single patient have the best day they could possibly have that day.”
And that’s a wonderful goal.

 Pediatric Palliative Care Helps Kids with Cancer Cope
Pediatric Palliative Care Helps Kids with Cancer Cope


 “In Case You Don’t Live Forever” by Ben Platt
“In Case You Don’t Live Forever” by Ben Platt
 Our Monthly Tip: Make an “In Case of Death” File to Ease Loved One’s Grief
Our Monthly Tip: Make an “In Case of Death” File to Ease Loved One’s Grief
















Its a really nice blog of cancer patients and also through it we got to know the challenges that take place while treatment. Thanks for such nice post.
Report this comment