
older Americans are experiencing more falls
Experts argue whether or not the over-prescription of certain medications could be the underlying cause of the increase in fall deaths.
Falls may seem like minor accidents, but for older adults in the United States, they are proving to be far more dangerous than most realize — even deadly. Recent statistics reveal that Americans over 65 are dying from fall-related injuries at higher rates than their peers in other parts of the world — a troubling trend with serious implications. A possible cause for this rise in fall-related deaths highlights the physical risks of aging, as well as gaps in prevention, support, and safety measures that could save lives.
In a recent opinion article published in the Journal of the American Medical Association (JAMA), one expert theorizes that the rise could be due to American’s over-reliance on prescription drugs. A corresponding article in the New York Times’ “The New Old Age” column calls that theory into question. Here’s what you should know:
The Statistics Regarding Fall-Related Deaths
Dr. Thomas Farley, an epidemiologist and public health expert, wrote the opinion article after noticing some startling trends in statistics. “In 2023, more than 41,000 individuals older than 65 years died from falls. Among older adults, the number of deaths from falls is more than from breast or prostate cancer, and is more than from car crashes, drug overdoses, and all other unintentional injuries combined,” he wrote, referencing the published statistics from the Center for Disease Control (CDC)’s Underlying Cause of Death database. Even worse, he noticed, was that the mortality rate for falls among older adults in the U.S. has more than tripled over the last 30 years.
Conversely, a recent analysis of global temporal trends and patterns in mortality from falls recently came to the conclusion that deaths due to falls decreased over the last 30 years in other high-income countries. So, what is happening in the United States that isn’t occurring overseas?
 Dr. Farley’s Hypothesis: Older Americans Are Over-Medicated
Dr. Farley’s Hypothesis: Older Americans Are Over-Medicated
As he is quick to admit, older adults have always been at risk for falls. The National Institute on Aging lists a number of contributing reasons for this tendency:
- Declining quality of eyesight, hearing, and reflexes
- Diabetes, heart disease, or problems with your thyroid, nerves, feet, or blood vessels can affect balance
- Conditions that cause rushed movement to the bathroom (such as incontinence)
- Mild cognitive impairment or certain types of dementia
- Age-related loss of muscle mass (sarcopenia), problems with balance and gait, and blood pressure that drops too much when you get up from lying down or sitting (postural hypotension)
- Foot problems that cause pain, and unsafe footwear
- Safety hazards in the home or community environment
- Some medications, or the combination of medications, especially those that cause side effects like dizziness or confusion.
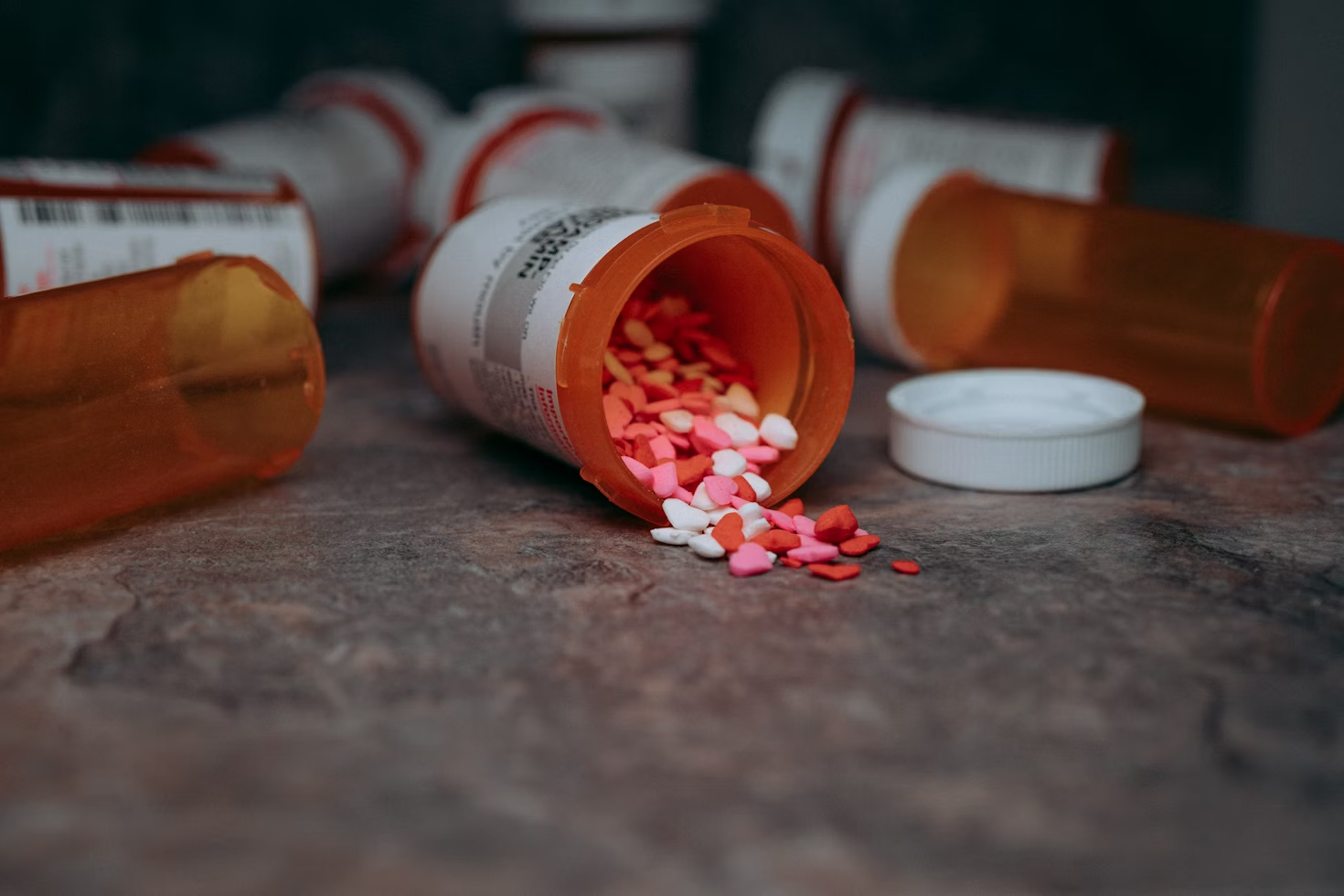
Knowing that most other countries have adults dealing with similar age-related conditions, Dr. Farley theorizes that our startling fall-related mortality rates must have to do with Americans’ tendency to overprescribe (and overuse) medications.
Older adults in the United States are heavily medicated. Citing a 2024 study investigating trends in prescription use, he wrote, “From 2017 to 2020, 90% of adults older than 65 years were taking prescription drugs, 43% were taking multiple prescription drugs, and 45% were taking prescription drugs that were ‘potentially inappropriate,’” he cites. Potentially inappropriate medications, or PIMs, are medications identified by the American Geriatrics Society’s (AGS) Beers Criteria “whose potential for harm outweighs their intended benefit in older adults.”
Many of these potentially inappropriate medications are drugs that cause drowsiness or impaired balance or coordination, also known as FRIDs, or fall risk-increasing drugs. Common FRIDs include opioids, benzodiazepines, gabapentinoids, antidepressants, beta-blockers, and anticholinergics. In addition to questioning the medical justification of the current prescription rates of many common FRIDs to older adults, Dr. Farley calls for more research in order to better understand the relative importance of different FRIDs in causing fall deaths.
Further complicating the issue, he goes on, is that many physicians (and patients) are reluctant to discontinue prescribed medications, even after a fall. A systematic review of the use of FRIDs and fall-related injuries, which found that many older adults who suffered a fall-related injury typically continued their use of FRIDs after the event, supported Farley’s claims. (The study states in its conclusion that “there is a need for well-designed interventions to reduce FRID use and falls in older adults with a history of falls.”)
Possible Alternative Explanations
As the New York Times points out, the same 30-year period that saw the dramatic increase in fall-related mortality rates was also a time when there was a flurry of research and government interventions designed to try and reduce geriatric falls. (The CDC’s STEADI program launched in 2019, and the United States Preventive Services Task Force started recommending exercise or physical therapy for older adults at risk of falling in 2012, 2018, and 2024, for example.)
While FRIDs are known to play a major role, geriatrician and epidemiologist at Yale University Dr. Thomas Gill told the Times that there are “alternative explanations” for the increase in death rates. One, he asserts, can be attributed to changes in how we report the cause of death. “Years ago, falls were considered a natural consequence of aging and no big deal,” he said. Death certificates often attributed fatalities among older people to ailments like heart failure instead of falls, making fall mortality appear lower in the 1980s and 1990s.
Additionally, the elongated life spans we are experiencing thanks to contemporary medicine means that there are more, older, frailer adults alive these days. Dr. Gill suggested that their accumulating impairments could make them more likely to die after a fall, as opposed to the drugs they may be taking for those impairments.
What the Experts Agree On
Whether or not prescription drug use outweighs all the other factors, “nobody disputes that these agents are overused and inappropriately used,” and contribute to the troubling increase in fall death rates among seniors, Dr. Gill told the Times.
In addition to the government’s continued attempted interventions — like the AGS’s recently published recommendations for alternative medications and nonpharmacological treatments — some experts have engaged in a campaign to “de-prescribe” FRIDs and PIMs for older adults as well.
Knowing that sometimes harried physicians might overlook possible risks when prescribing common FRIDs, the experts all recommend self-advocacy as the best method of avoiding preventable falls due to medications. “Ask, ‘Do any of my medications increase the risk of falls? Is there an alternative treatment?’” Dr. Steinman, co-chair of the Beers panel on alternatives, suggested. “Being an informed patient or caregiver can put this on the agenda. Otherwise, it might not come up.”

 More Older People Are Dying From Falls in the U.S.
More Older People Are Dying From Falls in the U.S.


 Final Messages of the Dying
Final Messages of the Dying
 Will I Die in Pain?
Will I Die in Pain?















